Measuring The Oral Microbiome in Saliva: Via a Covid Test Kit?

Microbes living on, and within our bodies, constitute one-to-two kilograms of our bodyweight, and contribute to how the body functions. Bacteria in your mouth interact with each other, and with you as their host – they assist digestion, can protect against pathogens, produce chemicals important for health, and they sometimes cause disease.
Depending on diet, general and oral health, microbiomes can be guardians or invaders, particularly of teeth and gums.
There are around 700 bacterial species found in the human mouth, and each of us is likely to be populated by around 300 various species.
Like its host, microbes need food; and it’s plentiful in the mouth. Saliva, what you eat, and the waste products of other microbes all nourish oral microbiome.
US researchers have found COVID-19 saliva testing kits that include a novel preservative can also be used to measure these microscopic organisms of the mouth. This enables further understanding of the relationship between mouth and lung microbes, and the SARS-CoV-2 virus (aka COVID-19) and opens the opportunity for new treatments being developed.
This Rutgers University study, published in NPJ Biofilms and Microbes is the first to test the accuracy of these saliva-based, at-home COVID test kits in measuring the oral microbiome. The journal is a platform for cross-disciplinary discussions that promote the quantifiable biology, ecology and communal function of biofilm populations and communities across the medical, environmental and engineering fields. It publishes applied science, as well as theoretical work of cell signalling and single cell interaction with human, animal and plant microbiomes, the natural environment, and any structure with which we live and interact.
Because we inhale a small amount of our saliva every day, it makes sense that some of the microbes that live in our mouths end up in our lungs.
It was found that the samples collected in the COVID testing kits still allowed for accurate measuring of bacteria, and gave a more stable illustration of microbiome over time, compared to kits without the preservative.
Researchers collected saliva samples from 22 participants. Six came back the next day to give another set of samples, allowing study of the microbiome over time.
Oral microbiome can show rapid change in composition and activity. Importantly, humans are developmentally dynamic – both spatially and sequentially – as the host. These multiplex, non-equilibrium motion and forces are the result of many factors: diet and host response to the changes in pH; interactions among the bacteria; and, across a longer time frame, gene mutations and horizontal gene transfer that bring new properties.
The symbiotic relationship between oral microorganisms is mutually beneficial. Commensal bacteria populations supply us, the host with essential nutrients while defending against opportunistic pathogens. They are involved in the development of intestinal architecture, and activations and suppression of processes, all in exchange for provision of nutrients, and a stable environment for the bacteria. Infection and disease occur when the commensal barrier is breached, and there is adherence to the mucosa. This is what makes bacteria pathogenic.
Health, or progression toward disease, is critically influenced by the microbiota that exists as a biofilm. Its crucial role is the maintenance of oral homeostasis, protecting the oral cavity, and preventing the development of disease.
Human microbial communities assist physiological, metabolic and immunological functions which include the generation of energy, differentiation and maturation of our immune system; control of fat storage and metabolic regulation; processing and detoxifying environmental chemicals; barrier function of skin and mucosa; balancing pro-inflammatory and anti-inflammatory processes; all in basic support of good health and prevention of disease.
Since 2008, recognising the importance of studying the human microbiome, the National Institute of Health has run the Human Microbiome Project (HMP). Recent developments in bioinformatics improve the ability to study human microbiome and the role of individual microbes in diverse ecosystems.
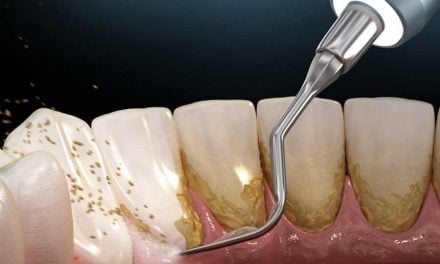
Similar to algae and barnacles that build up over the hull of a boat, our teeth and gums provide the perfect surfaces and environment for entire communities of microbes to exist.
This biofilm is consists of a range of microbes that like living together. While some bacteria are initial colonisers, others only move in when conditions are exactly right.

The bidirectional link between the brain, gut, and microbiome has moved to the forefront of research across the academic community over recent years. There is growing and multidiscipline evidence of the substantial link between healthy microbiome, particularly mouth and gut microbiota, and anxiety and depression.
Notably, studies have shown that prebiotics and probiotics effectively mitigate anxiety and depressive symptoms similarly to prescription medication, without side effects and with a general improvement in overall health. It makes sense. No matter how incrementally, when gut microbiome changes and becomes more balanced, signals to the brain differ, making better food choices becomes easier, digestion and micronutrient absorption occurs more easily and efficiently, sleep improves, motivation begins to return – and on goes that dynamic, domino effect.
With that, comes startling new research showing that with our modern diet, often based on convenience and speed with little consideration for seasonal foods and fresh variety, oral microbiome is becoming less diverse; with the follow-on being rapidly declining oral health across the richest countries in the world.
Such irony. Having the income to buy ecologically damaging, nutrient deficient food frequently enough for it to change the effect and proficiency of a vital and symbiotic physiological relationship that allows us to live, think and move. Makes you wonder how all that influences the world we live in, the world we create, and our response to the viruses in it. The viruses that move in when conditions are exactly right.
It’s understandable that the more severe the form of COVID-19, the higher the chance of complications like pneumonia, ARDS, sepsis, septic shock, and of course death. (The biggest shock.) The development, severity and risk of complications following a COVID-19 infection depend on a number of host and viral factors because it is these that affect immune response.
While 80% will have mild symptoms, 20% progress to a severe form of infection. It’s associated with higher levels of inflammatory markers, and an elevated bacteria and neutrophil-to-lymphocyte count.
The June 2020 British Dental Journal published a study suggesting the connection between the oral microbiome and COVID-19 complications should be investigated. The four co-morbidities associated with an increased risk of complications and death are also associated with altered oral biofilm, and periodontal disease: hence the important link. Periodontopathic bacteria are implicated in inflammation, bacteraemia, pneumonia and even death. It’s also present in severely infected patients. It is clear that bacterial superinfections are common in patients suffering from a severe case of COVID-19, prevalent in more than 50% of deaths. It’s common for respiratory viruses to predispose patients to bacterial superinfections. We would have learned that from the influenza outbreaks of 1918 and 2009, but despite the proven importance of superinfections in the severity of respiratory viral diseases, they remain understudied, because the complexity of diagnosis and culture-based microbiological testing becomes less scrutinised once the right antibiotics have been administered.
However it was discovered that for over 80% of ICU patients with an exceptionally high bacterial load, a dual regime of antiviral and antibiotic treatments proved successful.
Whether more research will be done on the connection of bacterial superinfections, oral microbiome and COVID-19 shouldn’t detract from the logic that dictates pre-existing oral disease – an already proven influence on heart disease – affects the severity and mortality risk of COVID-19.
So. Vaccine or no vaccine, maintain – if not improve – your oral hygiene. SARS-CoV-2 looks like it’s here to stay awhile, and it seems there’s the likelihood that eventually, everyone will get it. It’s not the virus that’ll kill you, it’s your response to it, so reduce bacterial load in the mouth to minimise the potential risk of a bacterial superinfection.
You know what to do. Brush and floss properly, eat healthily, and see your dentist. Improve what you eat, be aware of how you feel, notice how you think, and make conditions exactly right for some positive symbiosis between you and this present world.
DISCLAIMER:
The content has been made available for informational and educational purposes only. Northern Dental Design does not make any representation or warranties with respect to the accuracy, applicability, fitness, or completeness of the content.
The content is not intended to be a substitute for professional personal diagnosis or treatment. Always seek the advice of your dentist or another qualified health provider with any questions you may have regarding a dental or medical condition. Never disregard professional advice or delay seeking it because of something you have read or seen on the Site.