Dentistry & Eating Disorders: Helping With Detection & Care

Eating disorders are a terrible thing. Parents and loved ones who experience the destructive consequences of these modern scourges, often, find them heartbreaking. Today, we recognise eating disorders as serious illnesses, with psychological and physiological ramifications upon the health of individuals. Dentists can be the first port of call for those suffering from these potentially devastating conditions. Recognising the signs of an eating disorder is one of our responsibilities as dentists and health professionals.
The Dentist Identifying Eating Disorders
As clinicians, we are in the frontline for the detection of an eating disorder in our patients. We know, also, that early detection of an eating disorder can drastically improve the recovery chances of the individual. These conditions can affect people whatever their gender, age, and background. These are potentially life threatening illnesses and early intervention can save lives.
What Does An Eating Disorder Look Like?
They can involve eating too much and/or not eating enough. These conditions feature regular unhealthy and destructive eating habits. This can include restrictive dieting, compulsive eating, self-starvation, binge eating, self-induced purging, imbibing laxatives, and diet pills to name a few of the eating disorder manifestations commonly seen by dentists. You may be familiar with diagnostic names like Anorexia Nervosa, Bulimia Nervosa, and Binge Eating Disorder.
Who Is More At Risk of Developing an Eating Disorder?
It is important to remember that anyone can develop an eating disorder. However, children, adolescents, women, athletes, and those with a family history of eating disorders are at greater risk of developing the condition. Culturally, women have more pressure put upon them to appear a certain way in body shape terms. Women’s bodies are, also, more susceptible to life cycle transitions during puberty, pregnancy, and menopause.
Dentists & Oral Signs of Eating Disorders
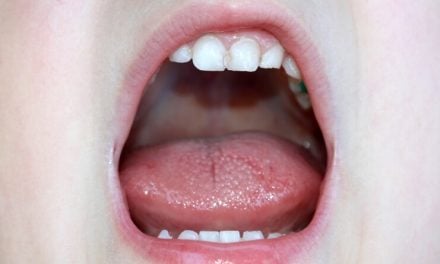
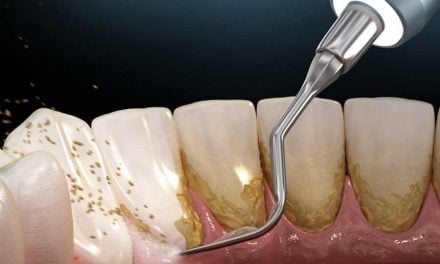
Peering into people’s mouths puts dentists in the box seat to observe the oral signs of these illnesses. Not eating enough and eating too much all leave tell tale signs for observant dental clinicians to recognise. There can be enamel erosion and erosive lesions present. Difficulty in swallowing is a red light warning in many instances. Sore throats, dry mouth, and burning tongue sensation are other signs to watch out for. Swollen salivary glands may be present. Mucosal legions and pharyngeal abrasions are further things to be aware of. Gum sensitivity and/or bleeding gingiva can be an indicator of issues related to eating disorders. The mouth is the portal where food is supposed to go in and neglect or overuse is, often, clearly apparent.
What Can a Dentist Do Once The Signs Are Recognised?
Initiating a discussion with the patient is the first step in providing care. Dental clinicians are best advised to point out the physical issues they have found and the long term consequences of leaving them untreated. Approach the situation in a non-judgemental way. Speak privately with the patient about the matter. Be positive and reassuring about future treatments to rectify the damage. Reinforce the message that the patient is not alone in dealing with this kind of thing. Provide the patient with information pertinent to their problems. Denial can be a common response for those with an eating disorder. Be patient and avoid being critical. Encourage patients to seek help where appropriate. Have reliable information on hand for referrals to eating disorder counsellors, psychologists, and clinicians. Establish an ongoing clinical relationship for the treatment of the oral and dental issues.
Dentists helping with detection and care is just another community service we are proud to carry out to help those in need. The pandemic has shown all of us what we can do to help each other and how good that is for our communities. Together we are stronger and more resilient.
Dentists and dental hygienists may see signs of eating disorders exhibited during routine visits, but without an arsenal of information and resources, they may not know the best way to direct patients to professional help or if they should intervene at all.
Dietary habits can and do play a role in oral health. Changes in the mouth are oftentimes the first physical signs of an eating disorder. The harmful habits and nutritional deficiencies that often accompany disordered eating can have severe consequences on one’s dental health.
An eating disorder may cause lingering or even permanent damage to the teeth and mouth. Early detection of eating disorders may ensure a smoother and more successful recovery period for the body and the teeth. Damage to the teeth and mouth can be tempered by arming yourself with the right information and receiving appropriate guidance from your oral health professional.

How Dentists Can Help With Detection & Care Of Eating Disorders
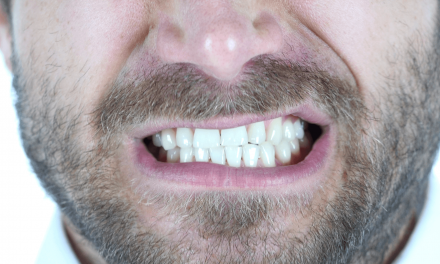
Often patients with eating disorders are embarrassed to see their dentist because of oral issues they may be experiencing. Bad breath, sensitive teeth, and tooth erosion are just a few of the signs that dentists use to determine whether a patient suffers from an eating disorder.
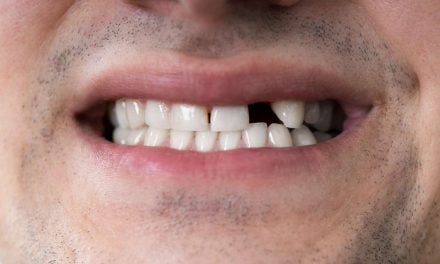
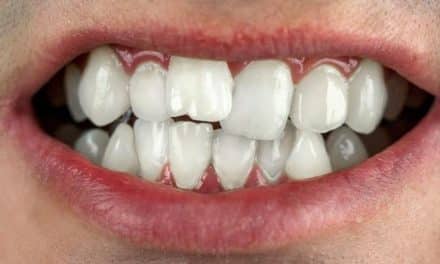
For those with bulimia, harsh stomach acid from frequent vomiting wears away tooth enamel increasing the risk of tooth decay; and the effects of anorexia, especially the lack of nutrients consumed, can weaken the jaw bone which also weakens teeth and leads to tooth loss.
Without the proper nutrition, gums and other soft tissue inside your mouth may bleed easily. The glands that produce saliva may swell. Individuals may experience chronic dry mouth.
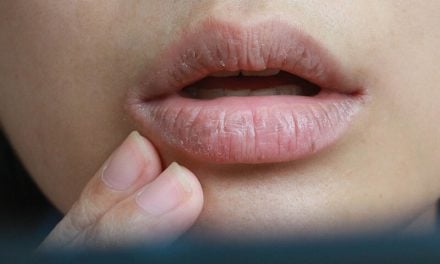
Food restriction often leads to nutritional deficiency. Nutrients that promote oral health include calcium, iron, and B vitamins. Insufficient calcium promotes tooth decay and gum disease; even if an anorexia patient does consume enough calcium, they also need enough vitamin D to help the body absorb it. Insufficient iron can foster the development of sores inside the mouth. Insufficient amounts of vitamin B3 (also known as niacin) can contribute to bad breath and the development of canker sores. Gums can become red and swollen almost glossy-looking which is often a sign of gingivitis. The mouth can also be extremely dry, due to dehydration, and lips may become reddened, dry, and cracked.
Frequent vomiting leads to strong stomach acid repeatedly flowing over the teeth. The tooth’s outer covering (enamel) can be lost and teeth can change in colour, shape, and length, becoming brittle, translucent, and weak. Eating hot or cold food or drink may become uncomfortable. Tissue loss and erosive lesions on the surface of the mouth may occur. The edges of teeth often become thin and break off easily. In extreme cases, the pulp can be exposed and cause infection, discolouration, or even pulp death. Tooth decay can be aggravated by extensive tooth brushing or rinsing following vomiting.
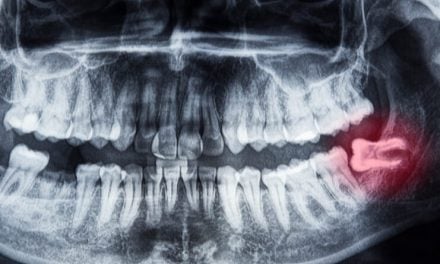
Degenerative arthritis within the temporomandibular joint in the jaw is a dental complication often associated with eating disorders. This joint is found where the lower jaw hinges on the skull. When arthritis begins in this joint it may create pain in the joint area, chronic headaches, and problems chewing and opening/closing the mouth.
Purging can lead to redness, scratches, and cuts inside the mouth, especially on the upper surface commonly referred to as the ‘soft palate.’ Such damage is a warning sign for dental professionals because healthy daily behaviors rarely cause harm to this area. Soft palate damage is often accompanied by cuts or bruises on the knuckles as a result of an individual’s teeth placing pressure on the skin while attempting to purge.
A frequent binge-and-purge cycle can cause an enlargement of the salivary glands. Enlarged glands can be painful and are often visible to others, which can lead to emotional distress.
Final Thought
Intervention by loved ones, friends, and medical and dental professionals can spur someone to seek eating disorder treatment. Early detection of the disease may ensure a smoother and more successful recovery period for the body and the teeth. Including a dentist in the health care team can help ensure that recovery is successful for the entire body. The key is to help direct individuals with an eating disorder in the direction of professional help, and that’s where the dentist near you can make a difference.
DISCLAIMER:
The content has been made available for informational and educational purposes only. Northern Dental Design does not make any representation or warranties with respect to the accuracy, applicability, fitness, or completeness of the content.
The content is not intended to be a substitute for professional personal diagnosis or treatment. Always seek the advice of your dentist or another qualified health provider with any questions you may have regarding a dental or medical condition. Never disregard professional advice or delay seeking it because of something you have read or seen on the Site.